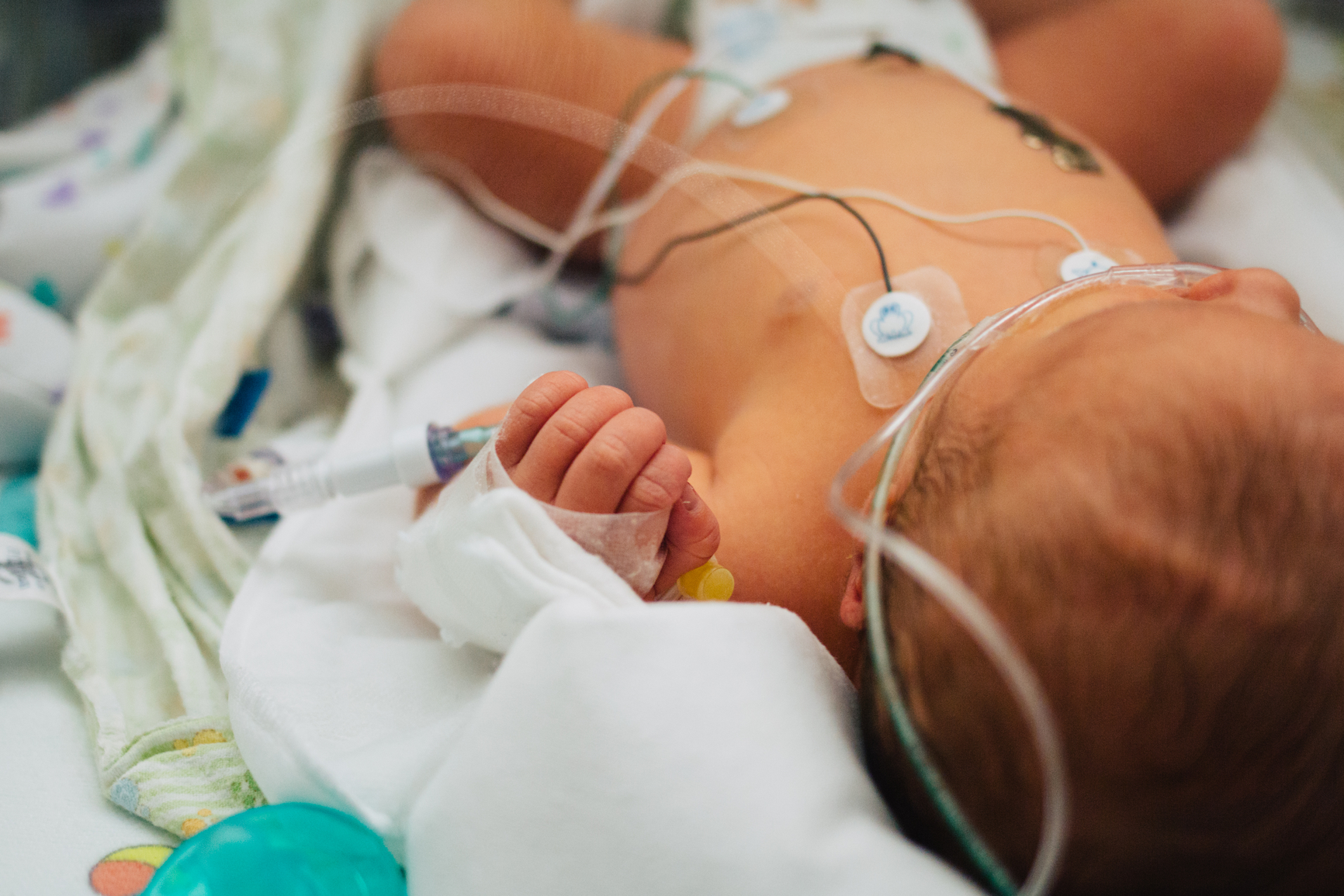
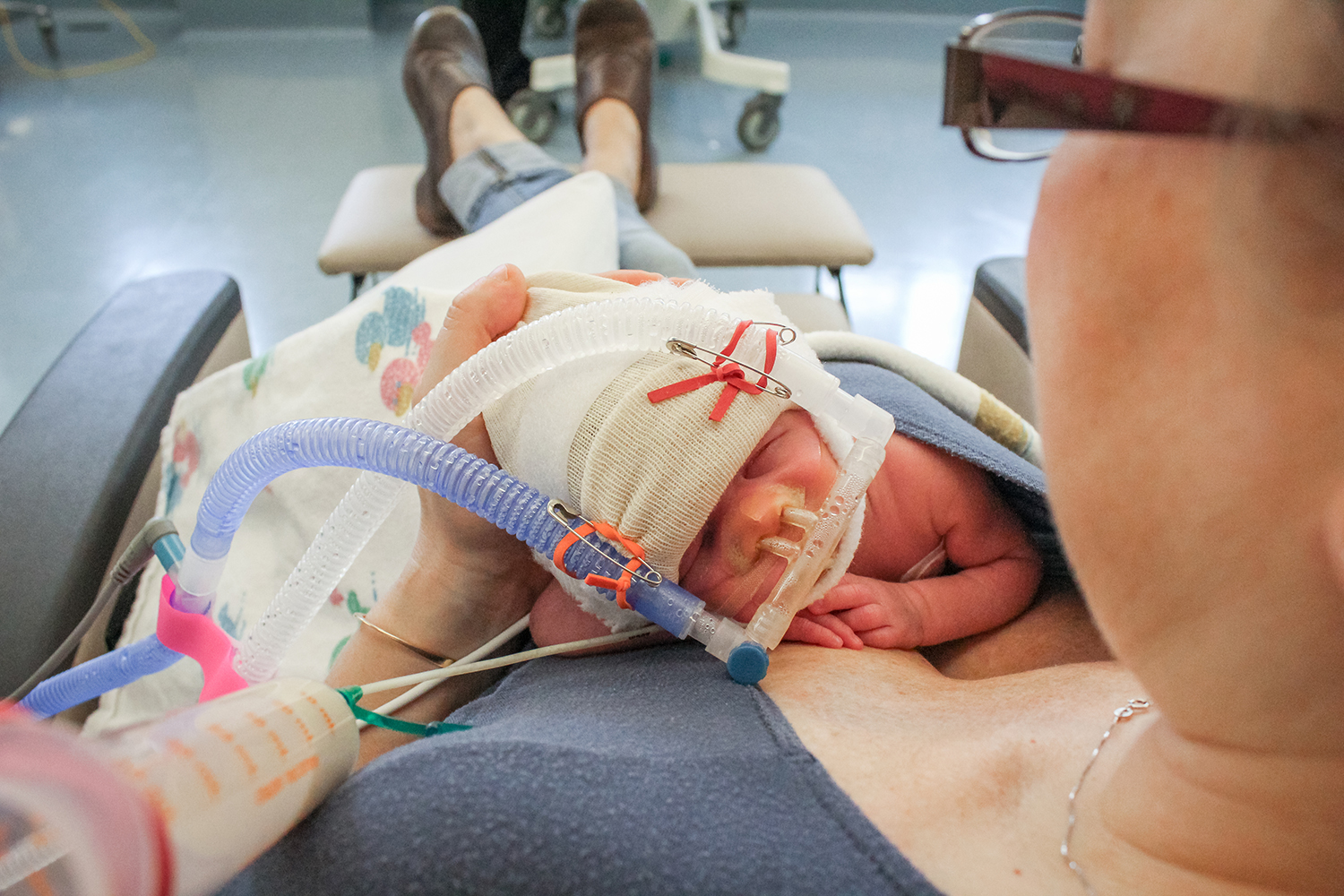
Cindy McEvoy, MD, MCR, is a physician-scientist at OHSU Doernbecher Children’s Hospital who specializes in infant lung health. The environment of the womb, along with the first weeks to months of life, sets the stage for our life-long lung health. Dr. McEvoy’s research focuses on improving lung function for preterm infants — even after they leave the hospital.
Dr. McEvoy is the Credit Unions for Kids Professor in Pediatric Research, director of maternal child health research in the department of pediatrics, and director of neonatal research. Her research helps to improve the standard of care for parents and their babies, so that all infants will have the best chance to breathe better for a lifetime.
What excites you about coming to work in the morning and what sort of projects are you working on right now?
My passion has always been translational and clinical research. It excites me to get up every day, walk through the nursery and interact with patients, and advance our knowledge of how to improve lifelong lung health.
I have several NIH projects that I’m working on right now looking at how we optimize the initial lung health of infants and children, and ultimately how that improves their lifelong lung health. One of the studies we are currently doing is an extended CPAP study. CPAP stands for continuous positive airway pressure, and many adults use this at night for sleep apnea. The CPAP helps to deliver positive pressure, and keeps a preterm baby’s fragile lungs from collapsing, and helps to stimulate the baby to continue to breathe on their own. One of our knowledge gaps is we don’t know how long we should leave a baby on CPAP if that preterm baby is now doing well. If I asked 100 different neonatologists when they would take a baby off CPAP, I might get 100 different answers.

This study randomizes infants to different durations of CPAP. We also employ pulmonary function tests during CPAP to see the effects this is having on their lung growth and development. We’re cautiously optimistic that we can help finetune how long a preterm baby should be left on CPAP. We’re not only seeing how well these babies are doing in the nursery, but we’re quantifying the effects after the babies go home until 6 months of age, which is one of the most important times for families.
Doernbecher is uniquely positioned for this because we are only one of two respiratory labs in the country who are able to use pulmonary function testing equipment in the nursery to quantify how baby responds to different interventions.
What are other collaborative projects you’re working on?
I am fortunate enough to be involved the Environmental influences on Child Health Outcomes (ECHO) consortium. This is a large trial supported by the NIH and is a fantastic example of team science. This study involves over 50 investigators like myself who have a number of birth cohorts and have been following children from birth to as late as their early 20s. It involves 50,000 moms and children followed from different time periods who we are studying under a common protocol.
As you can imagine, with this number of patients who have been followed this long, we are able to prospectively answer a number of questions about early life influences on a number of different outcomes. This includes my primary focus of respiratory outcomes, neurodevelopmental outcomes, weight and obesity trajectories, and the impact a variety of factors during pregnancy that may impact a child’s outcome. This study is across the U.S. and will be able to answer many important questions while also looking at geographical differences.
Why is this research so important to the health of an academic hospital?
Research motivates us to discover what’s new and coming in the future. Research continues to push us and the field of medicine forward. In the field of neonatology, we made tremendous strides since the first premature babies were supported through the development of different interventions, and now the mortality rate of very small babies is markedly decreased from when this field first started.
It’s critical to take problems we see at a patient’s bedside to the lab, and from the lab back to the patients and do these hypothesis-driven trials. I am thankful for support from places like Credit Unions for Kids to help support my career so I’m able to focus on patient care, hypothesis-driven trials and continuing to apply for grant support.
What is the importance of philanthropy to your work?
I can’t emphasize enough how important philanthropy is in general. Philanthropy has been important to my progress. I have been lucky to benefit from funding from the Friends of Doernbecher and funding through the Pratt Family Foundation, which supports our neonatology fellows and their projects.
Philanthropy can help invest in the next generation of physician-scientists which can be a very long road onto success. Support along the way is critical.
For instance, I received funding from the Friends of Doernbecher to obtain pilot data on our extended CPAP study. Then I was able to use that to apply for a large NIH grant, which likely would not have been successful without that initial investment from the Friends of Doernbecher. And it was even better, because with that support, one of our fellows in his training at the time also participated in the study and learned how to do hypothesis-generated research. This fulfilled his fellowship requirements, but we were able to publish this in a peer-review journal. The results have raised a lot of interest across the country of our ongoing trial.
I like to emphasize that sometimes a small amount of support can make such a huge difference in an individual’s career path. Philanthropy can help invest in the next generation of physician-scientists which can be a very long road onto success. Support along the way is critical.