Elizabeth “Liz” Powers, M.D., R ’06, M.H.A., was raised on the Upper Peninsula of Michigan by her family physician father and nurse practitioner mother. When they got snowed in, which was often, her father would snap on cross-country skis and head south to care for his patients at the community hospital in Iron River. In her family, obstacles were opportunities.
“I grew up understanding possibility,” says Powers. “That’s what my mom and my dad did for me — anything is possible. Look at it a different way.”
After completing a family medicine residency at OHSU in 2006, she and her husband, Nic Powers, moved to rural Enterprise in Eastern Oregon’s Wallowa County. She became the third physician partner at Winding Waters Clinic, a private primary care practice founded in 1972.
But Powers grew tired of sending patients home with a prescription and a referral to a specialist, only to learn — when she ran into them at the local Safeway — they’d taken a second job and then their car broke down, so they never made it to that other provider.
“When you’re a family physician, especially in a small community, you see how people actually live,” she says. “You are constantly confronted with the gaps — and a deepening sense of your own futility.”
Powers began studying the federally qualified health center (or FQHC) model, designed to bring comprehensive care to underserved areas. In 2015, Winding Waters became an FQHC Community Health Center.
That year, the health status of Wallowa County residents ranked 21st out of 36 counties in Oregon. By 2023, Winding Waters’ patient roster represented two-thirds of the county’s population. And Wallowa County had shot up the health rankings to eighth.
By looking at health care in a different way, Powers and her Winding Waters interdisciplinary team — including a half dozen other OHSU alumni — are joining kindred spirits across Oregon and the country in demonstrating the power and promise of this alternative approach.
Origin story
The path to better health in Wallowa County began 30 years ago when Enterprise physicians Lowell Euhus, M.D., and Scott Siebe, M.D., sounded the alarm about a worsening shortage of rural doctors.
From a summit they convened in 1989 came state funding for OHSU to launch Oregon’s Area Health Education Center (AHEC) and, eventually, the OHSU Campus for Rural Health. The goal: attract, train and retain health professionals committed to rural and underserved communities. In 1992, family medicine residents started rotating in Enterprise — and now students from across other OHSU schools do too.
Powers learned that origin story from OHSU family medicine physician and department chair John Saultz, M.D., who was at the 1989 summit with OHSU’s rural health education architect J.S. “Dutch” Reinschmidt, M.D. Tagging along with Saultz to an AHEC conference outside LaGrande in 2004 as a first-year resident, Powers was taken by his stories about rural Oregon and the meaningful role primary care doctors can play there.
“It was an Oregon history lesson,” she says, “from someone who really gets what it means to improve the health of a state.”
‘Look at it a different way‘
Powers graduated from Vassar College and Stanford Medicine, but it was in the OHSU family medicine residency where she found her people. After residency, it was in Wallowa County where she found her home.
With 7,500 residents spread across the northeast corner of the state, Wallowa is Oregon’s fifth least populous county. It’s a place of rugged beauty like the Upper Peninsula of Michigan where she could practice the kind of medicine her father did.
Except a lot had changed.
The fee-for-service model, where doctors get paid for each service provided, wasn’t keeping pace with the costs of care, particularly for primary care physicians. And the model emphasized the number of services rendered, not necessarily the quality or value to the patient.
Powers sought to flip that equation. Winding Waters signed on with the OHSU Oregon Rural Practice-based Research Network (ORPRN) to glean best practices. Powers and clinic leaders delved into the FQHC model.
Created in 1964, this model offers a generous, base-level of federal funding to clinics that deliver on a steep promise: sustaining advanced primary care services in underserved areas. In that broad mandate, front-line providers increasingly see the opportunity to offer — and get paid to provide — more comprehensive care that addresses the interrelated issues impacting people’s health.
Oregon-based innovations have helped. The state-funded Alternative Payment Methodology and Advanced Care Model pays for patient-centered, nontraditional services such as home visits, dental care coordination, transportation assistance, health education, counseling and more for people on the Oregon Health Plan (Medicaid). But Winding Waters wants to serve all comers. So they cobbled together a hybrid payor model.

Now, the approximately 5,300 patients that Winding Waters’ 105 team members see for medical care, dentistry, mental health counseling, substance use treatment and physical therapy each year are roughly evenly split between the Oregon Health Plan, private insurance and Medicare (for people with disabilities or over age 65). Nearly 10% have no insurance at all.
“It doesn’t matter who walks in the front door,” says Keli Dennis, chief operations officer for Winding Waters. “They could have a million dollars or zero dollars. They all get the same opportunity to have services.”
Interdisciplinary, team-based community care
The sun glints off the snowy mountains on a crisp March morning as patient Glenda Scott enters the Winding Waters Clinic in the small town of Wallowa — due west of Enterprise. The health center’s newest location features a community gathering space, pharmacy, full dental clinic, and medical and counseling offices.
For Scott, 70, a retired house painter and cleaner, the clinic’s wraparound services are helping her through the after effects of major heart surgery: managing multiple medications, recovering from significant weight loss and malnutrition, and navigating new functional limitations.
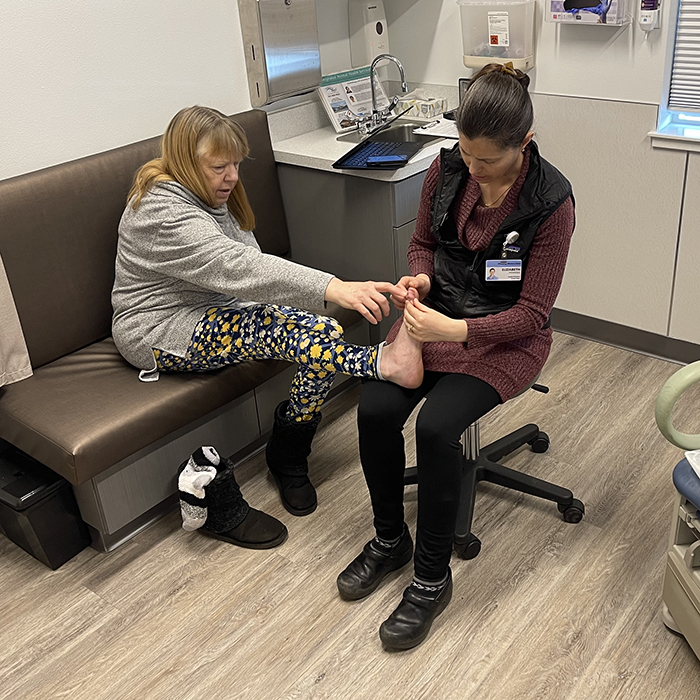
Powers sweeps into the exam room, brown hair pulled back in a messy bun, and greets the older woman with the warm smile of an old friend. She’s cared for Scott since she first started practicing.
At the end of the exam, she hands Scott off to a counselor who is helping Scott cope with anxiety. Powers’ interaction might have ended there. But, during the exam, she noticed evidence of poor circulation in Scott’s right foot and realized she was confused about her medications. So, Powers finds clinical pharmacist Michael Farley, R.Ph., in the team pod — the nerve center of the clinic — and Nathan Perren, a fourth-year student in the OSU-OHSU Pharm.D. Program rotating at the clinic.
“Mike, would you do me a favor?” Powers asks. “Would you go to her house and figure out what medications she’s taking?”
“It takes the whole to make you whole again. There’s physical, emotional, spiritual and mental. You can’t just do one of them.”
Amanda Raymond
Scott says such attentive care — which has also included home visits from a Winding Waters community nurse — has allowed her to remain at home where she, her daughter and her granddaughter, who is 23 and has a developmental disability, care for one another.
Scott’s daughter, Amanda “Mandy” Raymond, 50, adds that she’s gotten help at Winding Waters for her high blood pressure, chronic pain, migraines, depression and anxiety, as well as for substance use issues.
“It takes the whole to make you whole again,” Raymond says. “There’s physical, emotional, spiritual and mental. You can’t just do one of them.”
Anchored by alumni
The clinical leadership team at Winding Waters consists of nine department directors. Five are OHSU alumni.
Powers is chief medical officer and the health services officer responsible for integration of care. Nick West, M.D. ’19, R ’22, is quality director. Annika Maly, M.D., M.P.H. ’13, is integrated services director. Kevin Vandenheuvel, M.P.A.S. ’17, PA-C, is patient experience director. Joe Pierri, D.M.D. ’17, is dental director.
Family medicine physicians Wes Baker, M.D. ’14, R ’18, and Keith DeYoung, M.D., R ’09, also see patients. West is a product of Oregon’s and OHSU’s investment in rural health. He grew up on a ranch about an hour outside Enterprise. The state-funded Scholars for a Healthy Oregon Initiative helped pay his tuition in the OHSU M.D. Class of 2019 in exchange for rural service.
For West, embracing the integrated model at Winding Waters was natural.
“I recognized in med school that mental health is important, access to nutrition and dietary education are important, but I couldn’t allow the time during a 15-minute appointment,” he says. “We have all that right here and can leverage all our different specialties. While we do still have to refer out, it’s less than what we might need to because of our synergy.”
But for physicians like DeYoung and even Powers, who started out in the private-practice, referral-based model, the coordinated, interdisciplinary approach required a mental shift.
DeYoung says seeing how much patients like the integrated model helped. “And it’s just a lot more satisfying as a provider to actually give people the care they need,” he says.
Obstacles as opportunities
With the health of the whole community as their north star, Winding Waters has built social capital. They partnered with local nonprofits as well as the private community hospital, Wallowa Memorial.
Not everything, however, has gone their way.
In 2015, Winding Waters set out to launch a school-based health clinic in Enterprise to treat common ailments and also to ensure access to contraceptives. A small but vocal group of residents objected to any reproductive health care in a school. Winding Waters stepped back.
In 2018, the Wallowa County Board of Commissioners decided to transfer its local public health authority to the state and closed the public health department. Two years later, Winding Waters helped the county through COVID-19. The trust they built with their patients helped Wallowa County post impressive vaccination rates. Despite COVID-19 and a 6% increase in population, admissions at Wallowa Memorial Hospital between 2018 and 2023 dropped by nearly 23%, from 424 patients to 327.
By 2022, the Oregon Health Authority (OHA) could see the need to rebuild the county’s public health infrastructure. Seeking a local health officer, the OHA chose Powers.
A year later, when Landon Braden, superintendent of the Wallowa County Education Service District, needed partners to offer youth services in the ESD’s new Teen Drop-In Center in downtown Enterprise, he too turned to Powers. In the space of a month, Powers’ clinical team transformed an old office suite, a stone’s throw from the game room, into a welcoming, drop-in public health clinic.
At the grand opening on a sunny Friday in March, Powers gathers with Braden and her team in their gleaming clinic and gives each member a high five.
“I’m really hopeful for the community,” says Winding Waters quality manager Rachel Ellis.
“Yeah,” says Powers, flashing her wry smile. “We’re making progress.”
Fully accessible primary care
Oregon now has 32 FQHCs. Some, like Winding Waters, have multiple locations. And the safety net is growing, including the new OHSU Health Family Medicine, East Portland Community Health Center on the OHSU Health Adventist campus.
Policymakers and stakeholders are increasingly viewing the FQHC model — and ambitious interpretations like those at Winding Waters — as a salve for Oregon’s post-pandemic health care struggles.
“We are trying to address overlapping mental health, homelessness and fentanyl-abuse crises with a system that siloes physical health, mental health and substance use treatment,” says John McConnell, Ph.D., M.S., M.A., professor of emergency medicine and director of the OHSU School of Medicine’s Center for Health Systems Effectiveness.
“Nearly every level of care is swamped, and the emergency department (ED) has become the front door and holding pen,” he says. “If you start with comprehensive, interdisciplinary, fully accessible primary care for everyone, you can remove the stress on the ED and specialty care and give them space to do what they’re best at. We have much to learn from the FQHC model and pioneers like Winding Waters.”




