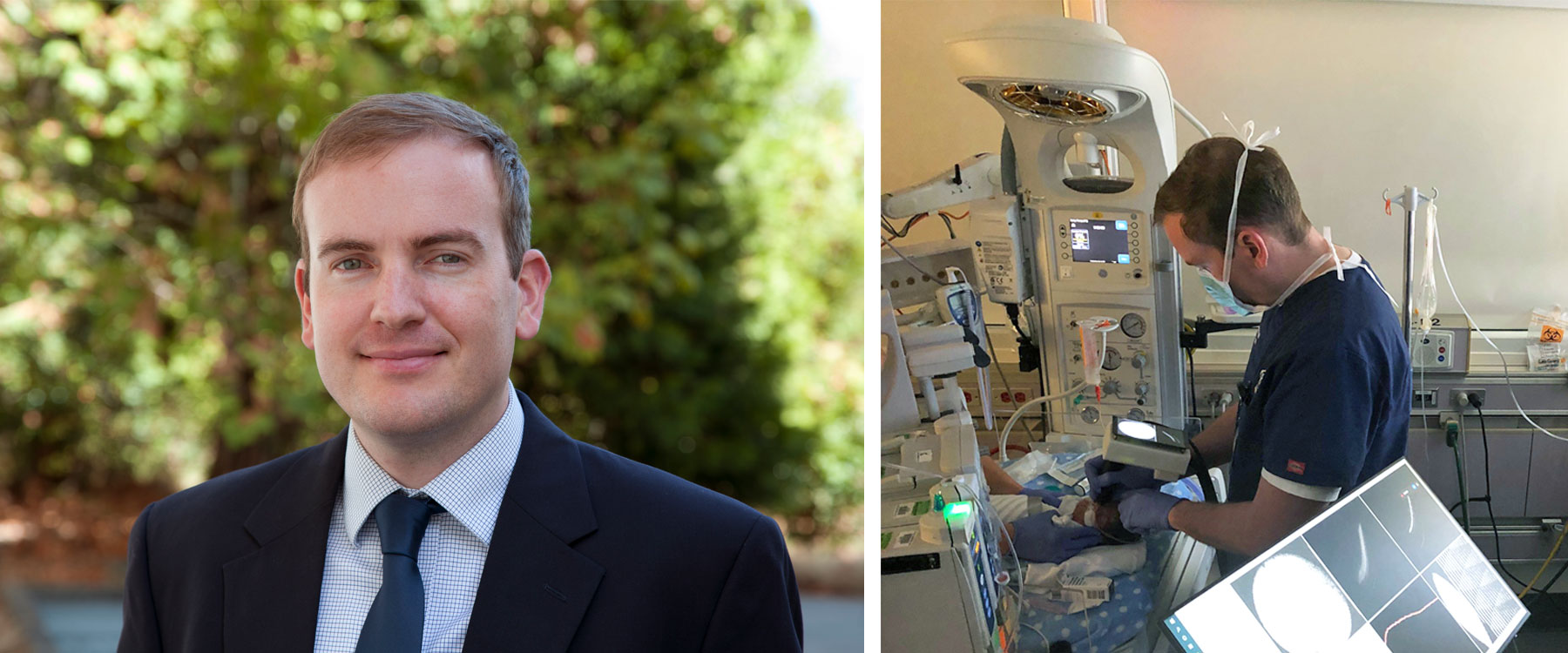
When the stakes are life and death, it takes a highly complex and coordinated sequence of care to save that child’s life. For the youngest of patients, like Penelope, that sequence often starts at a community hospital and concludes at OHSU Doernbecher’s Neonatal Intensive Care Unit, supported by telemedicine consulting and emergency transport.
Born blue
After an uneventful full-term pregnancy, Kristin Wise, of Oregon City, Oregon, was scheduled for induced labor and delivery at her local hospital. When Kristin’s contractions grew stronger and she neared the final stages of labor, the baby’s heartbeat suddenly disappeared. An ultrasound revealed that the umbilical cord was wrapped twice around the baby’s neck, pulling tighter with each contraction.
Kristin’s doctors raced her to the operating room for an emergency Cesarean delivery. Her husband, Tim, watched as the doctors rushed to revive his daughter, Penelope, who was blue and unresponsive.
“Our baby had been in cardiac arrest for 17 minutes,” Tim said.
The medical team went into full resuscitation mode, and soon monitors were beeping the good news of a functioning heart and lungs. But 17 minutes is a long time for the brain to not receive oxygen.
Kristin’s doctor contacted OHSU Doernbecher Children’s Hospital via a remote monitoring system that enabled Doernbecher neonatologists to see Penelope, check her vitals and advise.
Doernbecher’s neonatatology division chief Robert Schelonka, MD, said, “The telemedicine equipment includes a robotic camera that lets us zoom in to look at the patient and the room, assess everything going on, then provide the level of assistance that’s needed. In Penelope’s case, we knew we needed to immediately transport her to our NICU unit.”

Penelope and her parents were raced to Doernbecher by the Pediatric and Neonatal Doernbecher Transport, or PANDA. As the only certified patient transport for children requiring care in Doernbecher’s NICU, PANDA allows Doernbecher neonatologists to continually monitor the baby in transit with highly specialized technology, and prepare for her arrival.
Resuscitation efforts, telemedicine and specialized neonatal transport had saved Penelope so far. Now it was a matter of saving her brain: reducing swelling and preserving regular neurological development. Thankfully, baby Penelope was the perfect candidate for therapeutic hypothermia—a treatment that intentionally lowers the body’s temperature to preserve brain function.
When hypothermia saves lives
Hippocrates observed that infants exposed to the open elements survived much longer in winter than summer. Ancient Egyptians, Greeks and Romans cooled down their wounded soldiers after battle to protect them from brain damage. The positive effects of lowering body temperature have been studied and applied to all kinds of injuries for centuries.
Doernbecher’s NICU uses therapeutic hypothermia on infants to reduce brain swelling and the possibility of dangerous seizures. Medicated to reduce discomfort, the baby is placed atop a body-length cooling blanket. Over the next 24 hours, her temperature is lowered to 92.3 degrees Fahrenheit, where it is then held for 72 hours.
“Penelope was in an icy coma,” said Kristin, “and for three days, we could only sit with her and hold her tiny hand. She wasn’t responsive. Her hand was so cold, but we couldn’t put a blanket on her.
“The odds of her surviving were about 8 percent. It was surreal.”
“The odds of her surviving were about 8 percent. It was surreal.”
Kristin Wise, Penelope’s mom
The final 12 hours — the rewarming phase — is critical for babies like Penelope. Raising the temperature must be done slowly and incrementally, with close monitoring of blood pressure and other vitals, so that any issues can be addressed immediately.
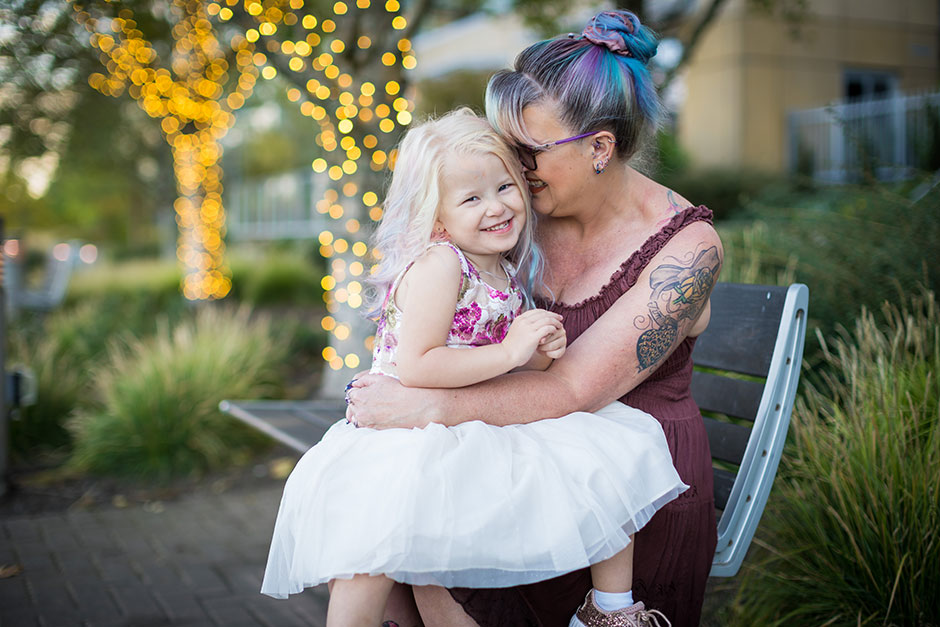
“This treatment,” said Nikki Wiggins, assistant nurse manager of Doernbecher’s NICU, “has to be done in an environment like Doernbecher, where we can provide a very high level of care with intense monitoring on advanced equipment, the ability to rapidly intervene, and subspecialty experts on staff.”
There are other hospitals in Oregon that offer therapeutic hypothermia, but Doernbecher has the most advanced brain monitoring for seizures. The monitoring is reviewed by a pediatric neurologist 24/7, from the time of admission until the baby completes treatment three days later—another distinguishing factor.
Penelope finally opened her eyes at six days old. She uttered her first cry at seven days old.
“Each felt like major milestones,” said Kristin. “The doctors were amazing—some of the most professional and caring people I have ever dealt with. The nurses didn’t just take care of Penelope, they also took care of me as I was recovering from my C-section, pumping breastmilk and managing the stress. We saw the compassion and quality of care the Doernbecher staff provide for all the families.”
“The nurses didn’t just take care of Penelope, they also took care of me.”
Kristin Wise, Penelope’s mom
Princess Penelope
After 11 days in the Doernbecher NICU, Penelope went home with her mom and dad.
“She was out of the woods within nine days,” remembered Kristin. “It was amazing. The doctor said she was a miracle. One nurse questioned whether she was looking at the right chart, because Penelope was doing so well.”
In the nearly four years since, Penelope has given her family many occasions to celebrate.

“Passing her cardiology and neurological follow-ups were huge,” Kristin said. “Walking at nine months.”
There have been a few scary situations, such as surgery to repair a small defect in her heart. And Penelope is delayed in her speech. Her parents know that the years ahead may reveal more issues, but for now their “Princess Penelope” is a typical, active and exuberant toddler.
With her mermaid-colored hair and glittery sneakers, Penelope is like a joyful little rainbow with energy to share. “She hugs everyone,” Kristin said. “Everywhere we go she wants to make friends. She loves every dog she encounters.”
Penelope loves the water, from pools to the bathtub to the ocean. Her laugh is infectious. She adores her older siblings, and enjoys singing to her favorite songs from the Disney movie Frozen.

Penelope — and countless other children — are alive today because of the level of highly specialized, team-oriented care at Doernbecher, services such as PANDA and telemedicine, and the generous support that makes that care and technology possible.
It is only through philanthropy that Doernbecher can ensure that such expert, comprehensive, leading-edge care is available around the clock. Whenever kids and their families need it.
No matter the odds.